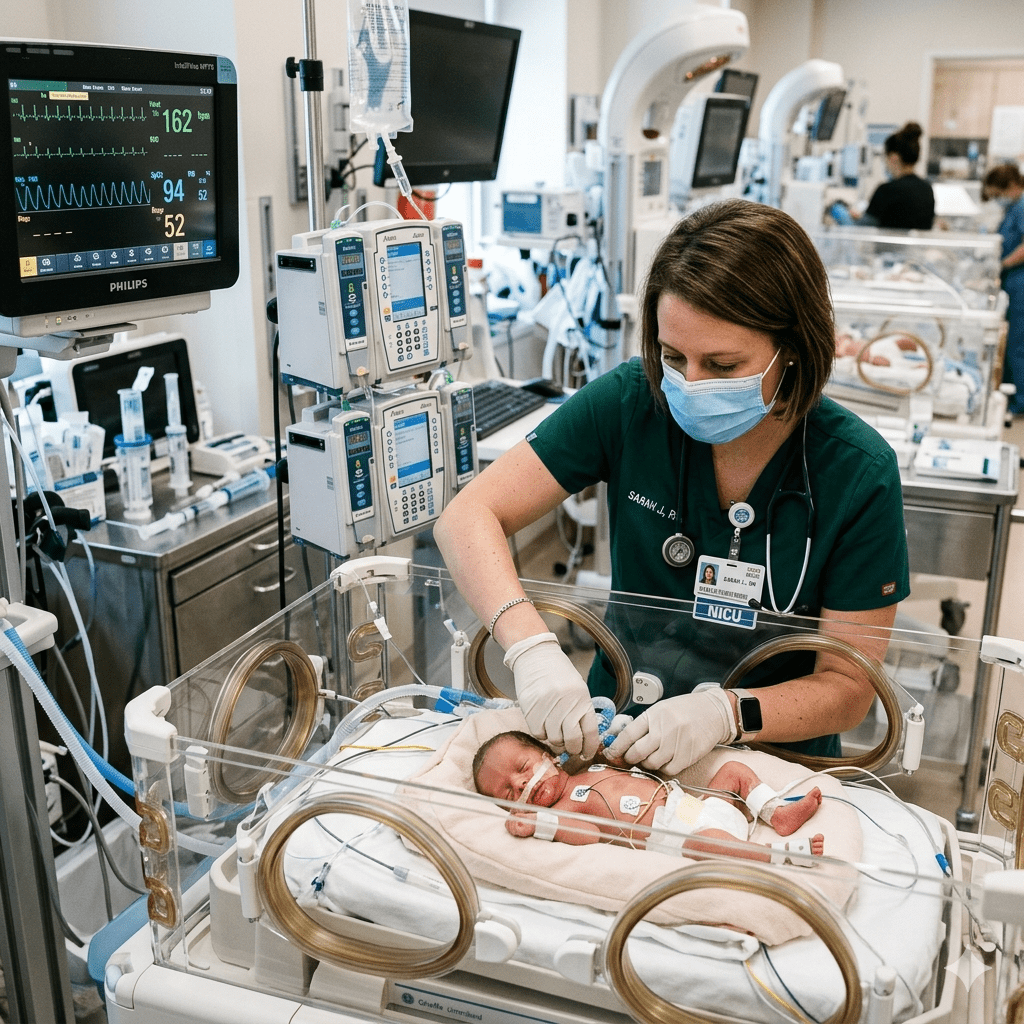
Neonatal sepsis remains one of the most life-threatening emergencies a registered nurse will encounter in the NICU or newborn nursery. Because newborns present with subtle, nonspecific signs, neonatal sepsis early detection requires a sharp clinical eye, sound knowledge of risk factors, and the ability to act swiftly before systemic deterioration occurs. For nursing students preparing for the NCLEX and practicing RN nurses alike, mastering this topic is non-negotiable — delayed recognition is directly associated with increased mortality and long-term morbidity.
Understanding Neonatal Sepsis: Definition and Classification
Neonatal sepsis is defined as a systemic bacterial, viral, or fungal infection occurring within the first 28 days of life. It is classified into two distinct categories based on timing of onset:
- Early-Onset Sepsis (EOS): Occurs within the first 72 hours of life. Most commonly caused by Group B Streptococcus (GBS) and Escherichia coli, transmitted vertically from mother to infant during delivery.
- Late-Onset Sepsis (LOS): Occurs between 72 hours and 28 days of life. More often linked to nosocomial pathogens such as Staphylococcus epidermidis, Staphylococcus aureus, Klebsiella, and Candida species, commonly associated with invasive devices like central lines or endotracheal tubes.
Every nurse working in maternal-newborn or pediatric settings must understand this classification, as it directly informs the likely causative organism, diagnostic approach, and empiric antibiotic selection.
Identifying Risk Factors: The Foundation of Early Detection
Neonatal sepsis early detection begins before the first clinical sign appears — it starts with identifying high-risk neonates at birth. Nursing assessment of maternal and neonatal risk factors is the first line of defense.
Maternal risk factors include:
- Prolonged rupture of membranes (PROM) — especially >18 hours
- Chorioamnionitis (intra-amniotic infection)
- Group B Streptococcus (GBS)-positive status without adequate intrapartum prophylaxis
- Urinary tract infection during pregnancy
- Fever during labor (≥38°C / 100.4°F)
- Preterm delivery (<37 weeks gestation)
Neonatal risk factors include:
- Prematurity and low birth weight (<2,500 g)
- Invasive procedures (central venous catheters, mechanical ventilation)
- Prolonged NICU hospitalization
- Immune immaturity — especially in preterm infants with immature humoral and cellular immunity
An RN nurse who routinely reviews the maternal history and flags these risk factors at admission creates an early-warning system that no lab test can fully replace.
Recognizing the Clinical Signs of Neonatal Sepsis
The hallmark of neonatal sepsis is its presentation with nonspecific, subtle signs — often described by experienced nurses as the infant simply “not looking right.” This clinical gestalt is important, but nursing practice demands systematic assessment.
Early signs to monitor closely:
- Temperature instability: Either hypothermia (<36.5°C) or fever (>38°C); hypothermia is more common in preterm neonates
- Respiratory changes: Tachypnea (>60 breaths/min), grunting, nasal flaring, retractions, or new oxygen requirement
- Cardiovascular instability: Tachycardia (>160 bpm) or bradycardia, poor perfusion, mottled skin, prolonged capillary refill time (CRT >3 seconds)
- Neurological signs: Lethargy, hypotonia, irritability, poor feeding, bulging fontanelle
- Gastrointestinal signs: Feeding intolerance, abdominal distension, vomiting, bloody stools
- Skin changes: Jaundice (especially early or rapidly progressing), pallor, petechiae, or purpura
These signs individually may be benign — together, or in the context of risk factors, they demand urgent nursing escalation. Use the SBAR communication framework when reporting concerns to the medical team to ensure complete and efficient handoff.
Diagnostic Workup: What the RN Nurse Must Know
Once sepsis is suspected, the nursing role pivots to facilitating a rapid and complete diagnostic workup — often referred to as the sepsis workup or sepsis screen.
Core laboratory tests include:
| Test | Clinical Significance |
|---|---|
| Complete Blood Count (CBC) | WBC <5,000 or >30,000/mm³ suggests infection; neutropenia is ominous |
| Immature-to-Total Neutrophil Ratio (I:T ratio) | >0.2 is significant; reflects bone marrow stress response |
| C-Reactive Protein (CRP) | Elevated (>10 mg/L) indicates systemic inflammation; rises 6–8 hours after onset |
| Blood Culture | Gold standard for diagnosis — must be drawn before antibiotic initiation |
| Lumbar Puncture (LP) | Performed when meningitis is suspected; CSF analysis and culture |
| Urinalysis and Urine Culture | More relevant in late-onset sepsis |
| Glucose | Hypoglycemia or hyperglycemia can accompany sepsis in neonates |
| Bilirubin | Early or exaggerated jaundice may indicate sepsis |
| Procalcitonin | Rises earlier than CRP; increasingly used as an adjunct biomarker |
The nursing priority is to obtain the blood culture from a peripheral site (not through existing lines if possible) before the first antibiotic dose — a contaminated or delayed culture compromises the entire diagnostic workup.
Nursing Interventions and Management of Neonatal Sepsis
Once neonatal sepsis is identified or strongly suspected, the registered nurse initiates and supports a series of time-sensitive interventions. Nursing bundles that address airway, circulation, and infection control within the first hour significantly improve outcomes.
Priority nursing actions:
- Notify the provider immediately — do not delay for additional assessment data if the infant looks unwell
- Obtain IV or IO access — peripheral IV or umbilical venous catheter (UVC) in neonates
- Administer empiric antibiotics as ordered — typically ampicillin + gentamicin for EOS; vancomycin ± gentamicin or cefotaxime for LOS
- Initiate fluid resuscitation cautiously — neonates are prone to fluid overload; monitor for signs of pulmonary edema
- Monitor vital signs continuously — attach cardiorespiratory monitor and pulse oximetry
- Maintain thermoregulation — use isolette or radiant warmer; correct hypothermia or hyperthermia
- Correct metabolic abnormalities — treat hypoglycemia (IV dextrose), monitor electrolytes and acid-base status
- Minimize handling — cluster care to reduce metabolic demand and stress
- Document — thorough, time-stamped nursing notes support continuity of care and NCLEX-style priority questions about documentation
Throughout the acute phase, the RN nurse serves as the constant monitor, the communicator, and the advocate — continuously reassessing for deterioration and ensuring the plan of care is executed precisely.
Prevention Strategies and Nursing Education
Prevention is a pillar of neonatal sepsis care. Nurses play a central role in implementing infection control measures that reduce the risk of both early and late-onset sepsis.
Key prevention strategies:
- Intrapartum GBS prophylaxis: Ensure penicillin or ampicillin is administered to GBS-positive mothers at least 4 hours before delivery; document timing accurately
- Hand hygiene: The most effective intervention against nosocomial late-onset sepsis — reinforce with all healthcare workers and families
- Aseptic technique: Strict sterile technique during central line insertion and maintenance; CLABSI bundles should be followed rigorously
- Breast milk promotion: Human breast milk provides passive immunity via secretory IgA; encourage and support breastfeeding or breast milk expression in the NICU
- Line care: Minimize catheter days; evaluate daily whether central lines are still needed
- Family education: Teach parents proper hand hygiene, signs of infection to watch for at home, and when to seek care after NICU discharge
These interventions are high-yield NCLEX content and core competencies for any nurse working in the neonatal or pediatric setting. Reference your nursing bundle study materials for a comprehensive breakdown of CLABSI and sepsis prevention protocols.
💡 NCLEX Tips for Neonatal Sepsis Early Detection
- Temperature instability in a neonate = sepsis until proven otherwise — hypothermia is more common than fever, especially in preterm infants
- Blood culture must always be obtained before the first antibiotic dose — this is a classic NCLEX priority question
- The I:T ratio >0.2 is a high-yield lab finding for NCLEX — it indicates left shift and sepsis risk
- A neonate who is lethargic, feeding poorly, and has a prolonged CRT meets clinical criteria for urgent sepsis evaluation — combine findings, don’t evaluate in isolation
- Empiric antibiotics for early-onset sepsis = ampicillin + gentamicin; know this drug combination and the rationale
Conclusion
Neonatal sepsis early detection is one of the most demanding clinical skills a nurse will develop — and one of the most rewarding when mastered. The ability to recognize subtle behavioral changes, interpret risk-stratified assessments, act before lab confirmation, and communicate urgently using SBAR distinguishes a competent RN nurse from an exceptional one. For nursing students and practicing registered nurses preparing for NCLEX or seeking to sharpen their clinical acumen, building fluency in neonatal sepsis recognition and response is an investment that directly saves lives.
Strengthen your neonatal and pediatric nursing knowledge by practicing with NCLEX-style questions at rn-nurse.com/nclex-qcm/ and explore comprehensive nursing bundles and courses at rn-nurse.com/nursing-courses/.