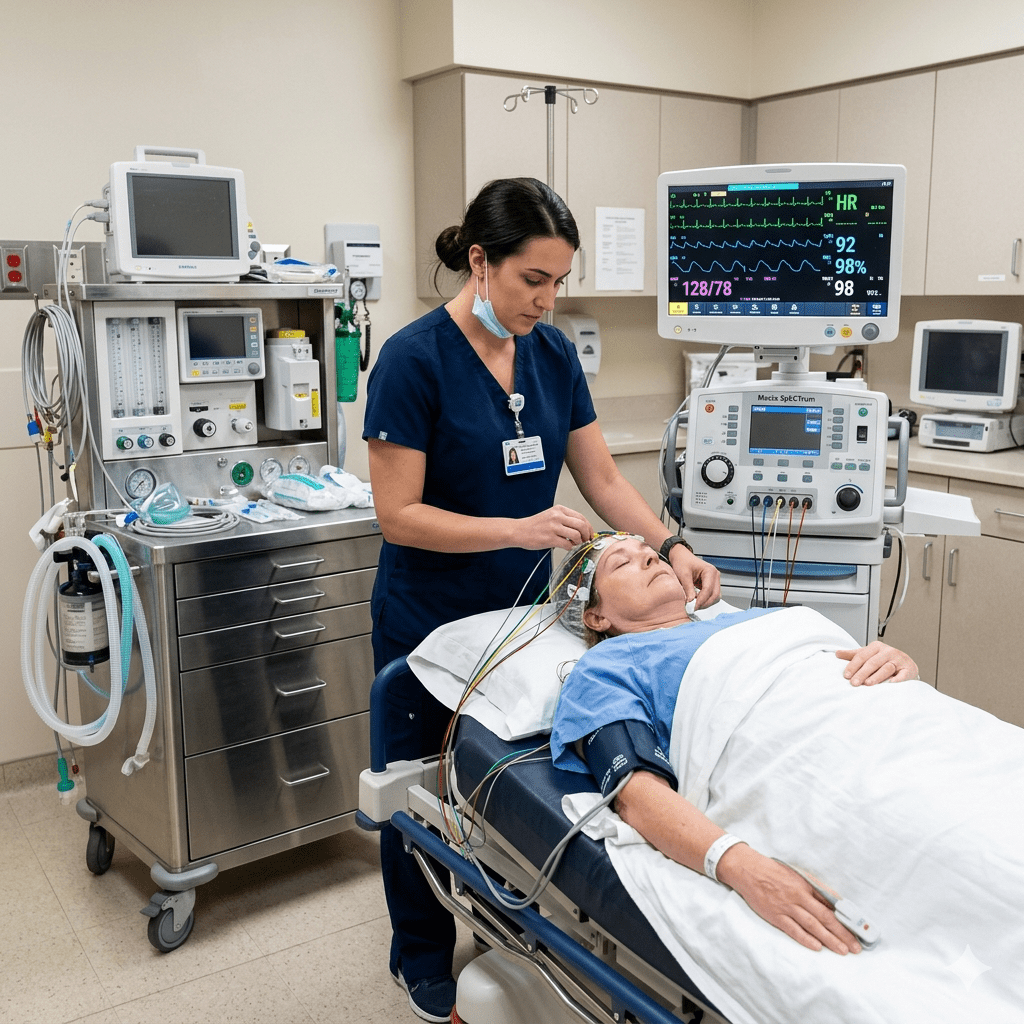
Electroconvulsive therapy (ECT) remains one of the most effective treatments for severe, treatment-resistant psychiatric conditions — yet it is also one of the most misunderstood procedures in mental health nursing. For the registered nurse working in psychiatric settings, understanding the full scope of the ECT nursing role is not optional. It is a clinical responsibility, and it is high-yield content for the NCLEX.
Whether caring for a patient with major depressive disorder (MDD), bipolar disorder with severe depression, or catatonia, the RN nurse plays a critical role at every phase of ECT treatment: before, during, and after. Mastering this content through a reliable nursing bundle sets the foundation for safe, evidence-based psychiatric care.
What Is ECT and When Is It Indicated?
Electroconvulsive therapy is a procedure in which controlled electrical currents are passed through the brain to intentionally induce a brief, generalized seizure. Performed under general anesthesia, ECT modifies neurotransmitter activity — particularly serotonin, dopamine, and norepinephrine — and has a rapid onset of therapeutic effect.
Primary indications for ECT include:
- Severe major depressive disorder unresponsive to pharmacotherapy
- Bipolar depression with psychotic features
- Acute suicidality requiring rapid symptom control
- Catatonia (particularly life-threatening forms)
- Schizoaffective disorder with prominent mood symptoms
- Postpartum psychosis
There are no absolute contraindications to ECT, but relative contraindications include recent myocardial infarction, intracranial mass lesions, and severe hypertension. The nursing team must communicate these risk factors clearly using SBAR before any procedure.
Pre-Procedure Nursing Responsibilities
Pre-procedure assessment and preparation represent a foundational part of the ECT nursing role. The registered nurse is responsible for both the physical and psychological readiness of the patient.
Pre-procedure nursing actions include:
- Obtain a complete nursing assessment: baseline vital signs, neurological status, cardiac history
- Confirm informed consent is signed — the nurse witnesses, does not obtain, consent
- Ensure NPO status for at least 6–8 hours before the procedure (aspiration risk under anesthesia)
- Remove dentures, jewelry, and hairpins before the patient enters the treatment room
- Establish IV access per facility protocol
- Administer pre-procedure medications as ordered — commonly atropine (to reduce secretions and prevent bradycardia) or a short-acting benzodiazepine antagonist if applicable
- Review the patient’s current medication list; lithium and clozapine may be held prior to ECT due to seizure threshold and cognitive risk
- Attach EEG leads, ECG electrodes, pulse oximetry, and blood pressure cuff
- Provide therapeutic communication — many patients experience significant anxiety about the procedure
The RN nurse must document baseline cognitive function using a validated tool (such as the MMSE) before the first ECT session. This data point becomes the reference against which post-treatment cognitive changes are measured.
The Nurse’s Role During ECT
During the ECT procedure, the nursing team works alongside anesthesia providers and the treating psychiatrist. The registered nurse monitors the patient continuously and is prepared to intervene rapidly if complications arise.
Intraoperative nursing responsibilities:
- Continuous monitoring of oxygen saturation, cardiac rhythm, and blood pressure
- Assist with airway management — the anesthesiologist administers a short-acting general anesthetic (commonly methohexital or propofol) followed by a muscle relaxant (typically succinylcholine) to prevent musculoskeletal injury during the seizure
- Observe and document the duration of the induced seizure — a minimum of 25 seconds is generally considered therapeutic; prolonged seizures (>120 seconds) require intervention
- Monitor the EEG tracing for seizure activity
- Ensure the bite block is properly placed to protect the airway and teeth
- Be prepared to manage post-ictal confusion as the patient emerges from anesthesia
Seizure activity during ECT is typically subtle due to muscle relaxants — the nurse may observe only minimal motor activity such as toe or ankle movement. This does not indicate treatment failure; EEG monitoring confirms the central therapeutic seizure.
Post-Procedure Recovery: Critical Nursing Interventions
The post-procedure phase is where the ECT nursing role becomes especially demanding. Patients emerge from anesthesia in a post-ictal state and require close monitoring and reorientation.
Post-procedure nursing priorities:
- Airway: Maintain a patent airway; keep the patient in a lateral recovery position until fully awake
- Vital signs: Monitor every 5–15 minutes until stable; watch for hypotension, tachycardia, and hypertension (autonomic stimulation is common immediately post-seizure)
- Orientation: Reorient the patient calmly and repeatedly — confusion, agitation, and short-term memory impairment are expected in the immediate post-ECT period
- Safety: Raise side rails; apply fall precautions; do not leave the patient unattended until alert and oriented
- Document: Record seizure duration, vital sign trends, level of consciousness, and any adverse events
Common short-term side effects the nurse must assess for and document:
- Headache — treat with acetaminophen per order
- Myalgia — muscle soreness from succinylcholine
- Nausea — administer antiemetics as ordered
- Confusion and short-term memory loss — reassure patient; this typically resolves between treatments
Cognitive Effects and Patient Education
Cognitive side effects are the most concerning aspect of ECT for patients and families. The RN nurse plays a central therapeutic role in managing these concerns through education and monitoring.
Short-term memory impairment is the most common cognitive side effect, and patients may experience anterograde (difficulty forming new memories) and retrograde (gaps in memories prior to ECT) amnesia. The nursing bundle for ECT education should address both types clearly.
Patient and family teaching points:
- Memory problems are temporary in most cases and typically resolve within weeks after completing the ECT course
- The number of treatments in a standard course ranges from 6 to 12 sessions, delivered 3 times per week
- Driving is prohibited on treatment days — the patient must have a responsible adult to provide transport
- The patient should not make major legal or financial decisions during an active ECT course
- Mood improvements may be noticed within the first 3–6 sessions
The registered nurse reinforces this education at every opportunity and supports the patient’s therapeutic communication needs. Many patients arrive fearful and benefit enormously from clear, honest, and compassionate explanations.
Quick Reference: ECT Nursing Overview
| Phase | Key Nursing Actions |
|---|---|
| Pre-procedure | NPO status, consent verification, IV access, baseline cognitive assessment, remove dentures/jewelry |
| During procedure | Airway monitoring, seizure duration documentation, vital signs, EEG observation |
| Post-procedure | Airway, reorientation, fall precautions, VS monitoring, side effect management |
| Patient education | Memory effects, transport needs, treatment schedule, when to expect improvement |
| Documentation | Seizure duration, VS trends, cognitive status, patient response |
💡 NCLEX Tips for ECT Nursing Role
- Priority post-ECT action: Maintain a patent airway — always the first nursing intervention after any procedure involving anesthesia.
- Consent: The nurse witnesses informed consent but never obtains it. This is the physician’s responsibility.
- Memory loss: Short-term memory impairment is expected and usually temporary. Do not minimize it, but reassure the patient it typically resolves.
- NPO: ECT requires NPO status for 6–8 hours. This is a safety measure due to general anesthesia and aspiration risk.
- Seizure duration: A therapeutic seizure lasts at least 25 seconds. Document the exact duration on the EEG.
Conclusion
The ECT nursing role is comprehensive, multiphase, and clinically demanding. From pre-procedure preparation and airway protection during treatment to post-procedure reorientation and ongoing patient education, the registered nurse is at the center of safe ECT delivery. Understanding each phase of care, the expected side effects, and the therapeutic communication skills needed to support patients through this process is essential for any RN nurse working in psychiatric settings.
For nursing students, ECT is high-yield NCLEX content — especially in the context of priority setting, patient safety, and therapeutic communication. Strengthen your readiness with targeted NCLEX practice questions at rn-nurse.com/nclex-qcm/ or explore the full nursing bundle of psychiatric nursing courses at rn-nurse.com/nursing-courses/ to build the clinical confidence you need on exam day and beyond.