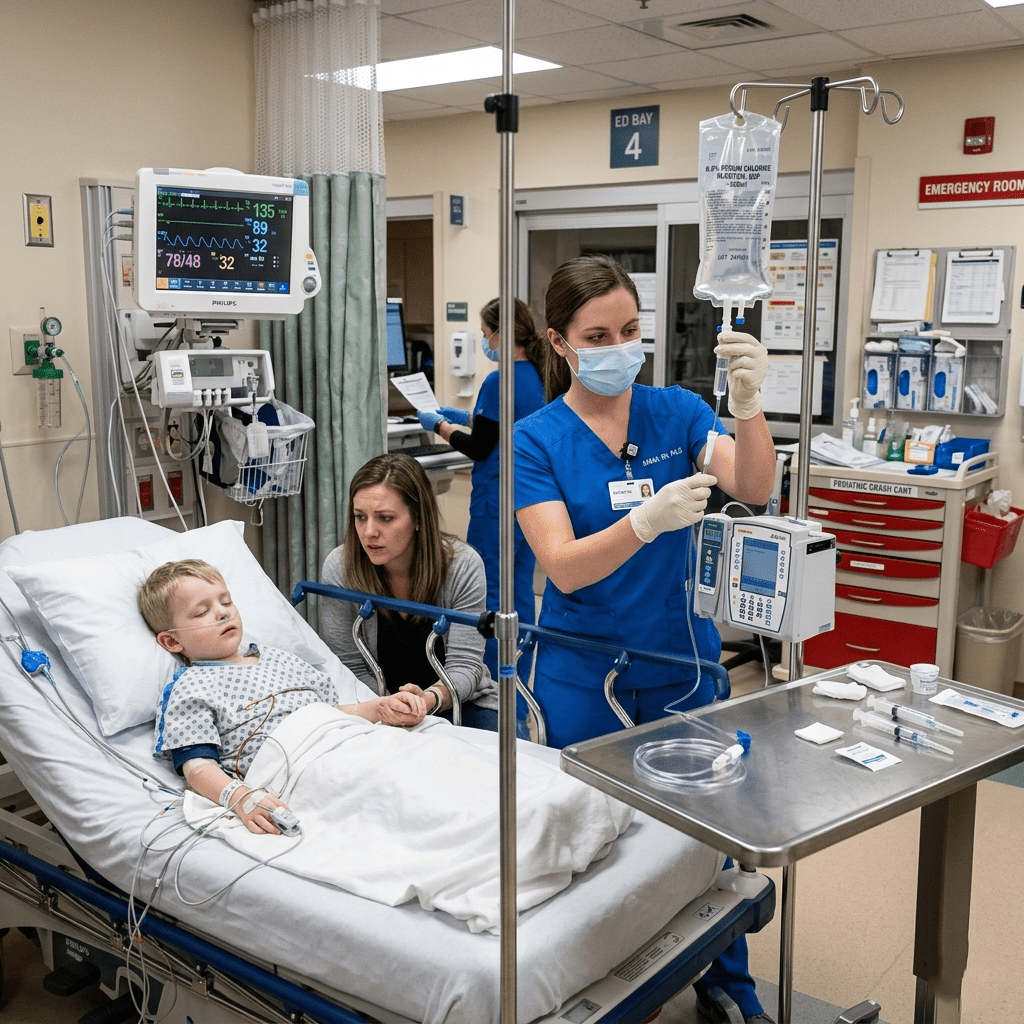
Shock in pediatric patients is a life-threatening emergency that requires rapid recognition and intervention. Unlike adults, children often compensate for shock until they suddenly deteriorate. Therefore, early assessment and immediate treatment are essential to prevent organ failure and death.
For every registered nurse, understanding pediatric shock is critical in emergency departments, pediatric units, and intensive care settings. This topic also appears frequently on NCLEX examinations, particularly in pediatric and critical care nursing questions. Additionally, hospitals often implement a structured nursing bundle for pediatric shock management to standardize assessment, fluid resuscitation, and patient monitoring.
This guide explains the different types of pediatric shock and the key differences in fluid resuscitation strategies, helping the RN nurse deliver safe and effective care.
What Is Pediatric Shock?
Pediatric shock occurs when the body cannot deliver enough oxygen and nutrients to tissues and organs. As a result, cells begin to fail and organ systems become compromised.
Shock can progress through several stages:
- Compensated shock
- Decompensated shock
- Irreversible shock
In the early stages, children often maintain normal blood pressure, which means that hypotension is a late and dangerous sign.
Because of this, the registered nurse must recognize early symptoms before blood pressure drops.
Early Signs of Pediatric Shock
Children in shock may present with several warning signs.
Common symptoms include:
- Rapid heart rate (tachycardia)
- Delayed capillary refill
- Cool or pale skin
- Weak peripheral pulses
- Altered mental status
- Decreased urine output
Recognizing these signs quickly allows the RN nurse to activate emergency treatment protocols and initiate rapid intervention.
Major Types of Pediatric Shock
Understanding the different types of shock helps guide treatment decisions and fluid management strategies.
Hypovolemic Shock
Hypovolemic shock is the most common type of shock in children. It occurs when the body loses significant fluid or blood volume.
Common causes include:
- Severe dehydration
- Vomiting and diarrhea
- Trauma and bleeding
- Burns
Because circulating volume is reduced, fluid resuscitation becomes the primary treatment.
Septic Shock
Septic shock occurs when a severe infection triggers widespread inflammation and circulatory collapse.
In pediatric patients, sepsis may develop from:
- Pneumonia
- Bloodstream infections
- Urinary tract infections
- Meningitis
Septic shock often causes abnormal blood vessel dilation and poor oxygen delivery, which requires aggressive treatment.
Cardiogenic Shock
Cardiogenic shock develops when the heart cannot pump blood effectively.
Common causes include:
- Congenital heart disease
- Myocarditis
- Cardiomyopathy
- Severe arrhythmias
Because the heart’s pumping ability is impaired, fluid resuscitation must be performed carefully.
Distributive Shock
Distributive shock occurs when blood vessels become excessively dilated, leading to poor blood circulation.
Examples include:
- Septic shock
- Anaphylactic shock
- Neurogenic shock
This type of shock often requires both fluids and medications to restore circulation.
Fluid Resuscitation in Pediatric Shock
Fluid resuscitation is one of the most important emergency interventions in pediatric shock.
However, the type and amount of fluids differ depending on the cause of shock.
Hypovolemic Shock Fluid Strategy
In hypovolemic shock, the primary problem is loss of circulating fluid volume.
Treatment typically includes:
- Rapid isotonic crystalloid fluids
- Initial fluid bolus administration
- Continuous reassessment of patient response
Because dehydration is the main cause, aggressive fluid replacement is often necessary.
Septic Shock Fluid Strategy
Septic shock requires rapid fluid administration combined with infection control.
Initial treatment may involve:
- Large fluid boluses
- Broad-spectrum antibiotics
- Vasopressor medications if needed
The RN nurse must closely monitor blood pressure, urine output, and oxygen saturation during treatment.
Cardiogenic Shock Fluid Strategy
In cardiogenic shock, excessive fluid can worsen heart failure and pulmonary edema.
Therefore, fluid administration must be carefully controlled and frequently reassessed.
Additional treatments may include:
- Inotropic medications
- Oxygen therapy
- Cardiac monitoring
Because of these risks, the registered nurse must observe respiratory status and signs of fluid overload.
Nursing Responsibilities in Pediatric Shock
The registered nurse plays a critical role in recognizing shock and implementing emergency interventions.
Key nursing responsibilities include:
Continuous Vital Sign Monitoring
Frequent monitoring of heart rate, blood pressure, oxygen saturation, and respiratory status is essential.
Rapid Fluid Administration
The nurse may administer emergency fluid boluses according to pediatric protocols.
Urine Output Monitoring
Urine output helps assess kidney function and circulation.
Early Recognition of Deterioration
Prompt communication with the healthcare team helps prevent complications.
Many healthcare facilities include these steps in a pediatric shock nursing bundle, which improves response times and patient outcomes.
Differences Between Adult and Pediatric Shock
Children respond differently to shock compared to adults.
Important differences include:
- Children maintain normal blood pressure longer
- Tachycardia is often the first warning sign
- Fluid needs may be weight-based
- Rapid deterioration may occur suddenly
Because of these factors, pediatric nurses must act quickly when early symptoms appear.
NCLEX Tips for Pediatric Shock
For NCLEX exam preparation, remember these important concepts:
- Hypovolemic shock is the most common pediatric shock type
- Hypotension is a late sign in children
- Fluid resuscitation often begins with isotonic fluids
- Nurses must monitor capillary refill, urine output, and mental status
Understanding these principles helps nursing students and RN nurses answer pediatric emergency questions correctly.
Conclusion
Pediatric shock is a medical emergency that requires rapid recognition and immediate treatment. Because children can compensate for shock longer than adults, early warning signs must never be ignored.
The registered nurse plays a vital role in identifying symptoms, administering fluid resuscitation, and monitoring patient response. Following structured nursing bundle protocols helps ensure consistent and effective treatment in emergency situations.
For both clinical nursing practice and NCLEX preparation, understanding the types of pediatric shock and the differences in fluid resuscitation strategies is an essential skill for every RN nurse caring for critically ill children.