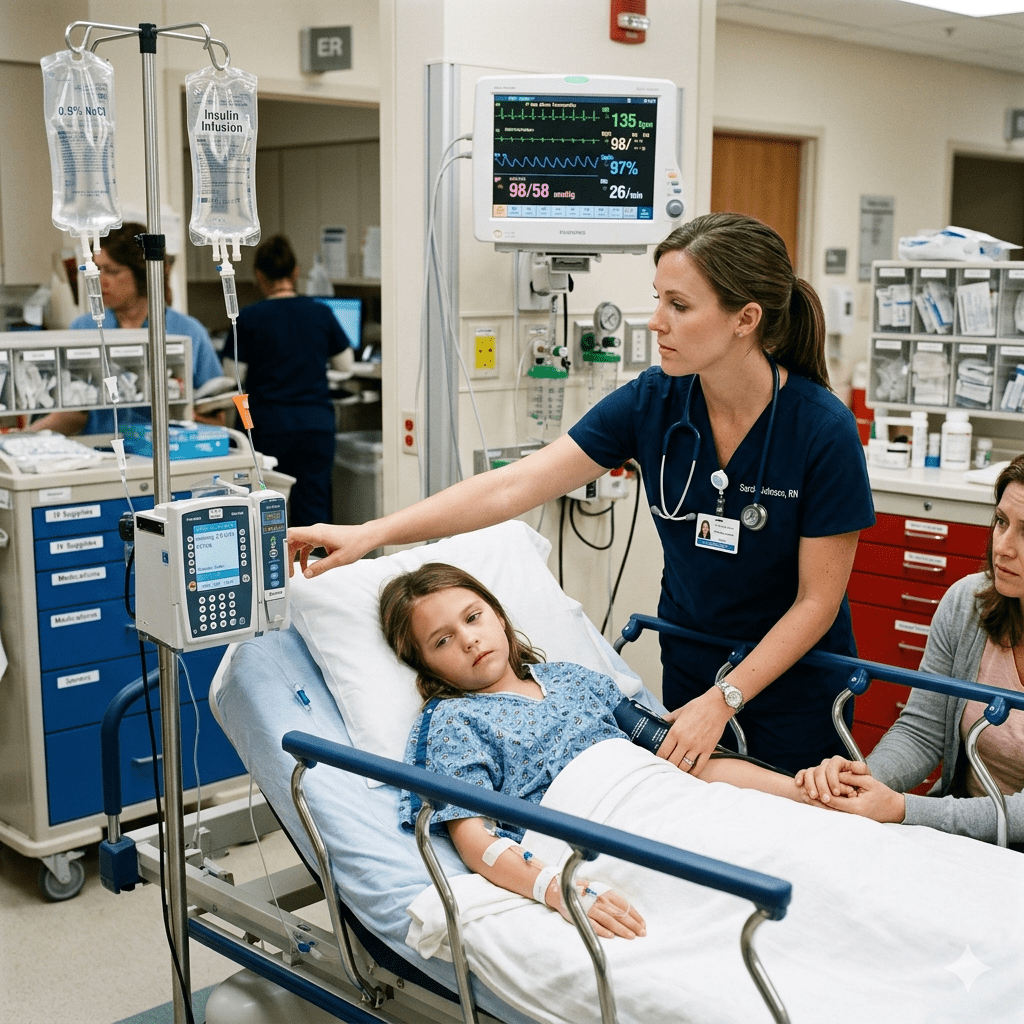Pediatric Diabetic Ketoacidosis (DKA) is a serious and potentially life-threatening complication of diabetes in children. It occurs when the body lacks enough insulin to use glucose for energy, forcing it to break down fat instead. This process produces ketones, which accumulate in the blood and lead to metabolic acidosis.
For every registered nurse, recognizing and managing DKA is essential because rapid treatment can prevent severe complications. In addition, pediatric DKA is a commonly tested concept on the NCLEX, making it important for every RN nurse and nursing student to understand the pathophysiology, assessment findings, and emergency nursing interventions.
Hospitals typically follow a structured DKA nursing bundle, which standardizes monitoring, fluid replacement, insulin therapy, and electrolyte management. Through careful assessment and coordinated care, the nurse plays a central role in stabilizing pediatric patients with DKA.
What Is Pediatric Diabetic Ketoacidosis?
Diabetic Ketoacidosis occurs when insulin deficiency leads to high blood glucose and ketone production. Without insulin, glucose cannot enter the cells, so the body begins breaking down fat for energy.
As fat metabolism increases, ketone bodies accumulate in the blood, causing metabolic acidosis and dehydration.
In children, DKA may develop rapidly. Therefore, early recognition by the registered nurse is critical to prevent complications such as cerebral edema.
Causes of Pediatric DKA
Several factors can trigger DKA in children with diabetes.
Common causes include:
- Missed insulin doses
- Infection or illness
- Undiagnosed type 1 diabetes
- Stress or trauma
- Insulin pump malfunction
In many cases, DKA is the first presentation of type 1 diabetes in pediatric patients. Because of this, nurses in emergency departments often encounter children who arrive with severe dehydration and metabolic disturbances.
Pathophysiology of DKA
Understanding the pathophysiology helps nurses provide safe care.
Three major processes occur during DKA:
1. Hyperglycemia
Insulin deficiency prevents glucose from entering cells. As a result, glucose accumulates in the bloodstream.
2. Ketone Production
The body breaks down fat for energy, producing ketones. Ketones are acidic, which leads to metabolic acidosis.
3. Severe Dehydration
High blood glucose causes osmotic diuresis, leading to excessive urination, electrolyte loss, and dehydration.
Because these processes occur simultaneously, DKA requires rapid intervention by the healthcare team and the RN nurse.
Signs and Symptoms of Pediatric DKA
Children with DKA may present with several distinctive symptoms. Early recognition is essential for effective nursing care.
Common symptoms include:
Early Symptoms
- Excessive thirst (polydipsia)
- Frequent urination (polyuria)
- Fatigue
- Weight loss
Progressive Symptoms
- Nausea and vomiting
- Abdominal pain
- Fruity or acetone breath odor
- Rapid breathing
Severe Symptoms
- Confusion
- Decreased level of consciousness
- Signs of shock
A key finding in DKA is Kussmaul respirations, which are deep and rapid breathing patterns that help the body eliminate excess acid.
The registered nurse must immediately report these findings to the healthcare provider.
Diagnostic Criteria for DKA
Healthcare providers diagnose pediatric DKA using laboratory values.
Typical findings include:
- Blood glucose >250 mg/dL
- Positive ketones in blood or urine
- Metabolic acidosis (low bicarbonate)
- Low arterial pH
Additionally, electrolyte abnormalities such as potassium imbalance often occur.
Continuous laboratory monitoring is therefore a critical part of the DKA nursing bundle.
Emergency Management of Pediatric DKA
Management focuses on fluid replacement, insulin therapy, and electrolyte correction.
The RN nurse plays a vital role in implementing these treatments safely.
Fluid Resuscitation
First, intravenous fluids are administered to correct dehydration.
Typically:
- Isotonic saline is given initially
- Fluids are adjusted gradually to prevent complications
Gradual rehydration is important because rapid fluid shifts may increase the risk of cerebral edema, a dangerous complication.
The nurse must monitor fluid balance carefully.
Insulin Therapy
Once fluids are started, continuous IV insulin infusion is usually initiated.
Insulin helps:
- Reduce blood glucose levels
- Stop ketone production
- Correct metabolic acidosis
The registered nurse must monitor blood glucose levels hourly to ensure safe insulin titration.
Electrolyte Monitoring
Electrolyte imbalances are common in DKA.
Important electrolytes to monitor include:
- Potassium
- Sodium
- Bicarbonate
Although potassium levels may appear normal initially, insulin therapy can cause rapid potassium shifts.
Therefore, the RN nurse must monitor cardiac rhythm and lab values closely.
Nursing Responsibilities in Pediatric DKA
Effective DKA care requires detailed and continuous monitoring.
Key nursing responsibilities include:
Frequent Vital Sign Monitoring
Vital signs should be checked regularly to detect signs of deterioration.
Neurological Assessment
Because cerebral edema is a major complication, nurses must assess:
- Level of consciousness
- Headache
- Behavioral changes
Blood Glucose Monitoring
Blood glucose levels are usually checked every hour during insulin therapy.
Strict Intake and Output Monitoring
Accurate measurement of fluid intake and urine output helps evaluate treatment effectiveness.
Using standardized protocols or a DKA nursing bundle helps ensure that every registered nurse follows evidence-based care.
Complications of Pediatric DKA
If not managed properly, DKA may lead to serious complications.
These include:
- Cerebral edema
- Hypoglycemia
- Electrolyte disturbances
- Acute kidney injury
Early recognition and rapid intervention by the RN nurse significantly reduce these risks.
NCLEX Tips for Pediatric DKA
For NCLEX preparation, remember these key points:
- DKA occurs due to insulin deficiency and ketone production
- Classic symptoms include polyuria, polydipsia, and Kussmaul respirations
- Treatment priorities include fluids, insulin, and electrolyte monitoring
- Nurses must watch for cerebral edema, the most serious complication
Understanding these concepts helps nursing students and registered nurses succeed on pediatric NCLEX questions.
Conclusion
Pediatric Diabetic Ketoacidosis is a critical emergency that requires rapid and coordinated care. Through careful assessment, laboratory monitoring, and prompt treatment, the registered nurse plays a key role in stabilizing pediatric patients.
Following structured protocols and a DKA nursing bundle ensures consistent treatment and improves patient outcomes. For both clinical practice and NCLEX success, mastering pediatric DKA management is essential knowledge for every RN nurse and healthcare professional involved in pediatric nursing care.