Edema is a common clinical finding that every nurse and registered nurse (RN nurse) must be able to assess, measure, and manage safely. It frequently appears in patients with heart failure, kidney disease, liver disorders, trauma, pregnancy, and post-surgical conditions. Because of its importance in patient assessment, edema is heavily tested on the NCLEX, making it a critical topic for nursing students and practicing nurses alike.
This article provides a clear, practical guide to understanding edema, measuring it accurately, and managing it effectively using evidence-based nursing interventions.
What Is Edema?
Edema is the abnormal accumulation of fluid in the interstitial spaces of the body. It occurs when fluid shifts from the intravascular space into surrounding tissues.
Common Causes of Edema
- Increased capillary pressure (heart failure)
- Decreased plasma proteins (liver disease, malnutrition)
- Increased capillary permeability (inflammation, trauma)
- Lymphatic obstruction (lymphedema)
- Sodium and water retention (kidney disease)
🔑 NCLEX Tip: Always think of edema as a fluid balance problem.
Types of Edema Nurses Must Recognize
Understanding the type of edema helps guide nursing care and treatment.
1. Peripheral Edema
- Affects feet, ankles, legs, arms
- Common in heart failure and pregnancy
- Often gravity-dependent
2. Pitting Edema
- Leaves an indentation when pressed
- Measured using a grading scale
- Common in cardiac and renal patients
3. Non-Pitting Edema
- No indentation when pressed
- Seen in lymphedema and hypothyroidism
4. Pulmonary Edema
- Fluid in the lungs
- Life-threatening emergency
- Symptoms include crackles, dyspnea, frothy sputum
🔑 NCLEX Focus: Pulmonary edema requires immediate intervention.
How Nurses Measure Edema
Accurate measurement is essential for monitoring patient progress and treatment effectiveness.
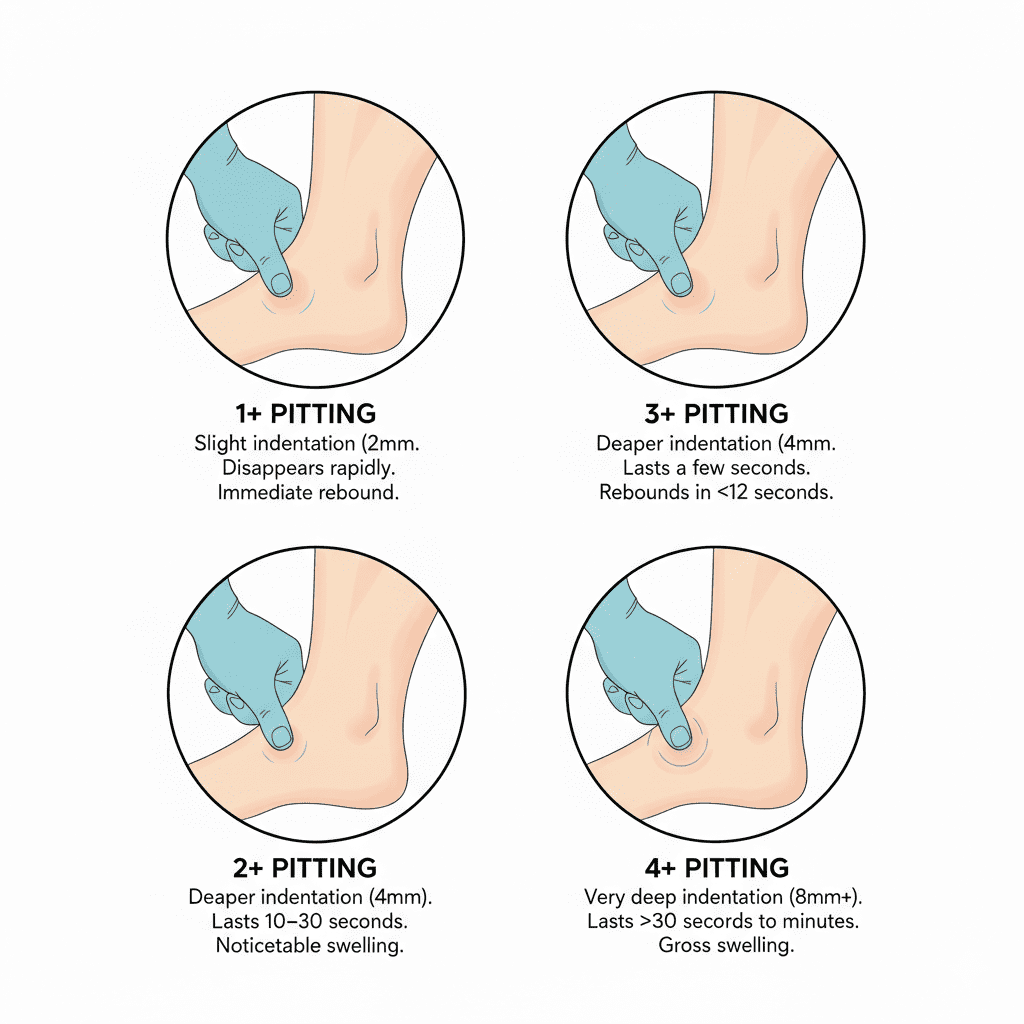
1. Edema Grading Scale (Pitting Edema)
| Grade | Description |
|---|---|
| 1+ | Slight indentation, disappears quickly |
| 2+ | Deeper indentation, rebounds in 10–15 seconds |
| 3+ | Noticeable indentation, rebounds in 1–2 minutes |
| 4+ | Severe indentation, rebounds in 2–5 minutes |
🩺 Nursing Tip: Always document location, grade, and symmetry.
2. Circumference Measurement
- Measure at the same anatomical point each time
- Use a tape measure
- Best for monitoring limb edema
📌 Example: Measure calf circumference 10 cm below the tibial tuberosity.
3. Daily Weights
- Most accurate indicator of fluid changes
- Same scale, same time, same clothing
- 1 kg (2.2 lb) ≈ 1 liter of fluid
🔑 NCLEX Alert: Sudden weight gain = fluid retention.
4. Intake and Output (I&O)
- Track fluids consumed and eliminated
- Especially important in renal and cardiac patients
Nursing Assessment of Edema
A comprehensive nursing assessment includes:
- Location and extent of edema
- Skin condition (shiny, tight, fragile)
- Pain or discomfort
- Vital signs
- Lung sounds
- Patient history (heart, kidney, liver disease)
👩⚕️ A skilled registered nurse correlates edema findings with the patient’s underlying condition.
Nursing Interventions for Managing Edema
1. Elevation
- Elevate affected limbs above heart level
- Reduces venous pressure
- Avoid prolonged dependency
2. Compression Therapy
- Compression stockings or wraps
- Promotes venous return
- Remove and assess skin regularly
⚠️ Contraindicated in severe arterial disease
3. Medication Management
- Diuretics (e.g., furosemide)
- Monitor electrolytes (especially potassium)
- Assess for dehydration and hypotension
🔑 NCLEX Tip: Loop diuretics → watch potassium levels.
4. Sodium Restriction
- Helps reduce fluid retention
- Educate patients on reading food labels
5. Skin Care
- Keep skin clean and dry
- Moisturize to prevent cracking
- Inspect daily for breakdown or infection
6. Mobility and Exercise
- Encourages circulation
- Prevents venous stasis
- Ankle pumps and ambulation are effective
Patient Education: A Key Nursing Role
Patient teaching improves outcomes and prevents complications.
Teach patients to:
- Elevate legs regularly
- Monitor daily weight
- Follow low-sodium diet
- Take medications as prescribed
- Report sudden swelling or shortness of breath
📚 These concepts are reinforced in many nursing bundle study guides designed for NCLEX preparation.
NCLEX-Style Practice Question
A patient with heart failure has 3+ pitting edema in both ankles. What is the nurse’s priority intervention?
A. Encourage increased fluid intake
B. Elevate the legs above heart level
C. Apply heat to the ankles
D. Massage the swollen areas
✅ Correct Answer: B
Rationale: Elevation reduces venous pressure and promotes fluid reabsorption.
Common NCLEX Traps About Edema
- ❌ Focusing only on swelling, not the cause
- ❌ Ignoring daily weight changes
- ❌ Massaging severe edema
- ❌ Applying compression without checking circulation
Why Edema Management Matters for Nurses
Effective edema management:
- Prevents skin breakdown
- Improves mobility
- Reduces respiratory complications
- Indicates treatment effectiveness
For every RN nurse, edema assessment is a core clinical skill that reflects strong nursing judgment.
Final Thoughts
Measuring and managing edema is a foundational nursing skill that connects anatomy, physiology, assessment, and patient care. Whether you are a nursing student preparing for the NCLEX or a registered nurse in clinical practice, mastering edema assessment improves patient outcomes and exam success.