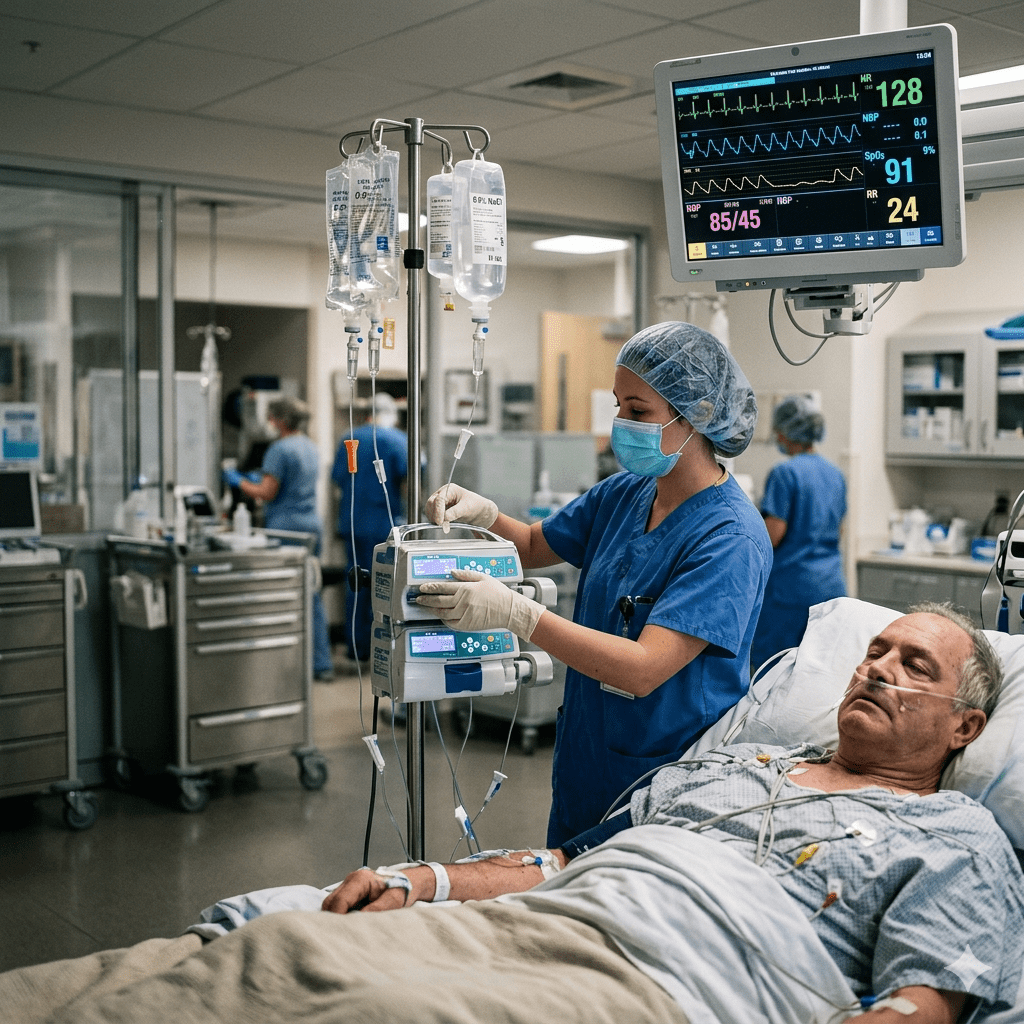
Septic shock is a life-threatening medical emergency that requires rapid intervention to restore circulation and prevent organ failure. One of the most important treatments is fluid resuscitation, which helps improve blood pressure, tissue perfusion, and oxygen delivery. Because this condition progresses quickly, every nurse and registered nurse (RN nurse) working in emergency or intensive care settings must understand effective fluid resuscitation strategies.
In modern healthcare, early recognition and aggressive management of septic shock are critical. Therefore, fluid therapy is often initiated within the first hours of diagnosis. These principles are widely taught in critical care nursing programs and frequently appear in NCLEX exam preparation materials. In addition, many educational resources and nursing bundle study guides highlight sepsis protocols to help future nurses develop strong clinical decision-making skills.
This article explains septic shock, why fluid resuscitation is necessary, and the strategies used to manage this serious condition safely.
What Is Septic Shock?
Septic shock is a severe form of sepsis, a systemic infection that causes widespread inflammation and circulatory instability. During septic shock, blood vessels dilate and become more permeable. As a result, fluid leaks into surrounding tissues, causing a drop in blood pressure and reduced blood flow to vital organs.
Patients with septic shock may experience:
- Persistent hypotension
- Rapid heart rate
- Fever or hypothermia
- Decreased urine output
- Altered mental status
- Elevated lactate levels
Because these symptoms indicate poor tissue perfusion, immediate treatment is necessary.
For the RN nurse, recognizing these warning signs is essential for initiating early sepsis protocols and improving patient outcomes.
Why Fluid Resuscitation Is Essential
Fluid resuscitation is one of the first treatments used to stabilize patients with septic shock. The goal is to restore circulating blood volume and improve oxygen delivery to the body’s organs.
During sepsis, blood vessels become abnormally dilated and fluid shifts out of the bloodstream into tissues. Consequently, blood pressure drops and organs may not receive enough oxygen.
Administering intravenous fluids helps:
- Increase circulating blood volume
- Improve cardiac output
- Restore tissue perfusion
- Stabilize blood pressure
Because early treatment improves survival rates, rapid fluid administration is a key priority in emergency and critical care nursing.
Initial Fluid Resuscitation Guidelines
Most clinical guidelines recommend administering rapid intravenous fluids during the early stages of septic shock.
A common recommendation is:
30 mL per kilogram of crystalloid fluids within the first three hours.
Crystalloid solutions commonly used include:
- Normal saline
- Lactated Ringer’s solution
These fluids help restore circulation and support cardiovascular stability.
The registered nurse plays a vital role in initiating fluid therapy, monitoring infusion rates, and observing patient response.
Monitoring Patient Response to Fluids
Although fluid resuscitation is essential, excessive fluids can lead to complications. Therefore, careful monitoring is required to determine whether the patient is responding appropriately.
Important indicators include:
- Blood pressure improvement
- Increased urine output
- Improved mental status
- Decreasing lactate levels
- Better peripheral perfusion
The RN nurse continuously monitors these parameters to evaluate treatment effectiveness.
In some cases, advanced monitoring techniques may also be used to assess fluid responsiveness.
Balanced vs Normal Saline Solutions
In recent years, clinicians have discussed the benefits of balanced crystalloids compared with normal saline.
Balanced solutions, such as lactated Ringer’s, more closely resemble the body’s natural electrolyte composition. These fluids may reduce the risk of complications such as metabolic acidosis.
However, both types of fluids remain widely used in septic shock management.
The nurse must understand the differences between these solutions and monitor patients for potential electrolyte imbalances.
When Fluids Are Not Enough
Sometimes fluid resuscitation alone cannot stabilize a patient with septic shock. If blood pressure remains low after adequate fluids, additional treatments may be required.
These may include:
- Vasopressor medications (such as norepinephrine)
- Oxygen therapy or mechanical ventilation
- Antibiotic therapy to treat infection
- Source control procedures to eliminate infection
The registered nurse works closely with physicians and the critical care team to monitor patient status and support these interventions.
Risks of Excessive Fluid Administration
Although fluids are essential in septic shock treatment, giving too much fluid can cause complications.
Possible risks include:
- Pulmonary edema
- Respiratory distress
- Increased cardiac workload
- Tissue swelling
Because critically ill patients are vulnerable to fluid overload, the RN nurse must carefully assess patient response and report any concerning changes.
Balancing fluid administration and patient safety is a critical responsibility in advanced nursing practice.
Nursing Responsibilities in Septic Shock Management
The nurse plays a central role in managing septic shock. Continuous monitoring and early intervention are essential for improving patient outcomes.
Key responsibilities include:
- Recognizing early signs of sepsis
- Initiating sepsis protocols
- Administering IV fluids rapidly
- Monitoring vital signs and perfusion
- Tracking urine output
- Communicating patient changes to the healthcare team
These tasks require strong clinical judgment and careful observation.
Because septic shock can deteriorate rapidly, the registered nurse must remain vigilant at all times.
Importance for NCLEX Preparation
Sepsis and septic shock management are major topics in modern nursing education. As a result, fluid resuscitation strategies frequently appear on the NCLEX exam.
For example, test questions may ask the RN nurse to:
- Identify early signs of septic shock
- Determine priority interventions
- Recognize appropriate fluid therapy strategies
- Monitor for complications of fluid resuscitation
Understanding these concepts helps students develop the clinical reasoning skills required for safe patient care.
How Nursing Study Bundles Support Learning
Critical care topics such as septic shock can be complex for many students. Structured learning resources like a nursing bundle help simplify these important concepts.
A well-designed nursing bundle often includes:
- Sepsis management flowcharts
- Fluid resuscitation guidelines
- Critical care nursing checklists
- NCLEX-style practice questions
These resources allow future registered nurses to review key information quickly and effectively.
Final Thoughts
Septic shock is a life-threatening condition that requires immediate treatment to prevent organ failure and death. Fluid resuscitation is one of the most important early interventions used to restore circulation and improve tissue perfusion.
Because nurses are often the first healthcare professionals to recognize patient deterioration, they play a critical role in initiating and managing fluid therapy. The RN nurse must carefully monitor patient response, prevent complications, and collaborate with the healthcare team to ensure effective treatment.
For students preparing for the NCLEX, mastering fluid resuscitation strategies is an essential part of critical care nursing education. With continued practice and the support of organized study resources like a nursing bundle, future registered nurses can develop the knowledge and confidence needed to manage septic shock successfully.