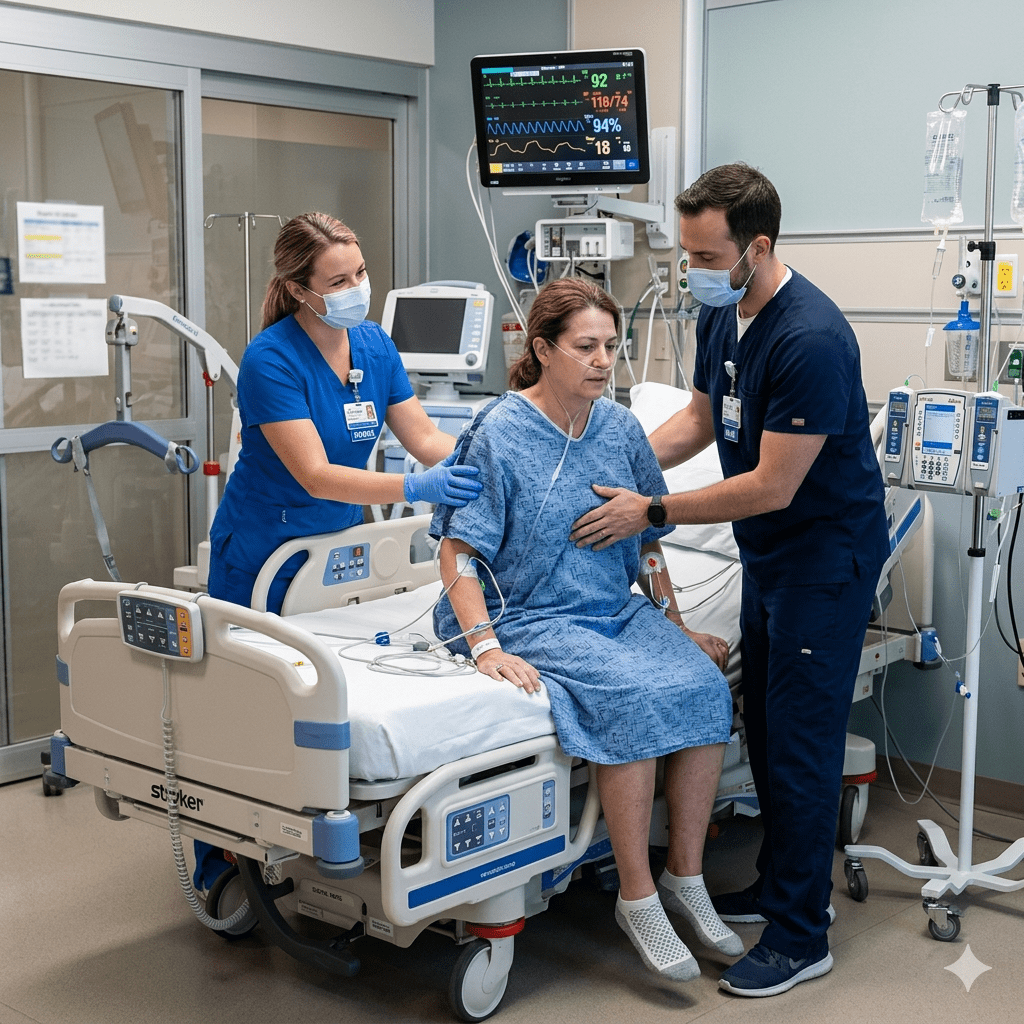
Early mobility programs are becoming an essential part of modern critical care. Traditionally, patients in the intensive care unit (ICU) were kept on prolonged bed rest. However, research now shows that early movement and physical activity can significantly improve recovery outcomes. Therefore, every nurse and registered nurse (RN nurse) working in critical care should understand the importance of early mobility in ICU patients.
These programs focus on safely initiating movement and rehabilitation activities as soon as a patient becomes medically stable. Because mobility directly affects recovery, it is frequently discussed in advanced nursing education and may also appear in NCLEX exam questions. Additionally, many study guides and nursing bundle resources highlight early mobility protocols to help nursing students understand modern ICU care practices.
This article explores what early mobility programs are, their benefits, and the critical role nurses play in implementing them.
What Are Early Mobility Programs?
Early mobility programs are structured plans designed to encourage safe movement and physical activity in critically ill patients as soon as possible during their ICU stay.
Instead of waiting until patients are fully recovered, healthcare teams now begin mobility interventions while the patient is still receiving treatment. Consequently, patients can regain strength and physical function more quickly.
These programs may include activities such as:
- Passive range-of-motion exercises
- Sitting at the edge of the bed
- Standing with assistance
- Walking short distances with support
Each activity is carefully adjusted based on the patient’s medical condition.
For the RN nurse, understanding the stages of mobility progression helps ensure patient safety and effective rehabilitation.
Why Early Mobility Is Important in the ICU
Critically ill patients often experience rapid muscle loss due to immobility. Even a few days of bed rest can lead to significant muscle weakness and functional decline.
Early mobility helps prevent several complications associated with prolonged bed rest, including:
- Muscle atrophy
- Pressure injuries
- Blood clots
- Delayed recovery
- Reduced lung function
Because of these risks, modern critical care emphasizes early rehabilitation whenever possible.
The registered nurse plays a key role in identifying when patients are stable enough to begin mobility activities.
Benefits of Early Mobility Programs
Implementing early mobility programs provides several benefits for ICU patients.
Improved Muscle Strength
Movement stimulates muscle activity and helps maintain strength. Therefore, patients who participate in early mobility programs often experience less severe weakness during recovery.
Reduced ICU Length of Stay
Patients who regain strength earlier may recover faster and leave the ICU sooner. This improvement benefits both patient outcomes and healthcare systems.
Better Respiratory Function
Physical movement encourages deeper breathing and improved lung expansion. Consequently, early mobility may reduce complications such as pneumonia.
Improved Mental Health
Critically ill patients may experience anxiety, confusion, or delirium. Engaging in physical activity and interacting with caregivers can improve mental well-being.
Because of these benefits, early mobility is now considered a standard component of many ICU care protocols.
Stages of ICU Mobility
Early mobility programs usually follow a gradual progression based on the patient’s medical stability and physical ability.
Stage 1: Passive Movement
At this stage, the patient may still be sedated or unable to move independently. Healthcare providers perform passive range-of-motion exercises to maintain joint flexibility.
The nurse assists by positioning the patient properly and ensuring safe handling during exercises.
Stage 2: Active Bed Exercises
Once the patient becomes more alert, they may begin performing simple movements such as lifting arms or bending knees while in bed.
The RN nurse monitors vital signs and patient tolerance during these activities.
Stage 3: Sitting and Standing
As the patient gains strength, the healthcare team may help the patient sit on the edge of the bed or stand with assistance.
This stage requires close supervision to prevent falls and monitor cardiovascular stability.
Stage 4: Assisted Walking
Finally, patients may begin walking short distances with support from nurses or physical therapists.
Walking helps rebuild muscle strength and improve circulation.
Nursing Responsibilities in Early Mobility Programs
The registered nurse plays a critical role in implementing early mobility safely.
Key nursing responsibilities include:
- Assessing patient readiness for mobility
- Monitoring vital signs before and during activity
- Assisting with safe patient transfers
- Preventing falls or injuries
- Communicating patient progress with the healthcare team
Because ICU patients may have multiple medical devices, such as ventilators or IV lines, careful coordination is essential during movement.
The nurse must ensure all equipment remains secure while assisting the patient.
Safety Considerations During Mobility
Although early mobility has many benefits, safety must always be the top priority.
Before initiating movement, the RN nurse should assess:
- Blood pressure stability
- Oxygen saturation levels
- Level of consciousness
- Presence of medical devices or lines
- Overall patient strength
If the patient shows signs of distress, activity should be stopped immediately.
Close monitoring ensures that mobility remains beneficial rather than harmful.
Importance for NCLEX Preparation
Early mobility and prevention of immobility complications are important topics in nursing education. Because these principles relate directly to patient safety, they frequently appear in NCLEX exam questions.
For example, the registered nurse may be asked to:
- Identify complications of prolonged bed rest
- Determine appropriate mobility interventions
- Prioritize patient safety during transfers
- Monitor patient response to activity
Understanding these concepts helps nursing students develop strong patient care skills.
How Nursing Study Bundles Support Learning
Many nursing students benefit from structured study resources when learning complex ICU concepts.
A comprehensive nursing bundle may include:
- ICU mobility protocols
- Patient positioning diagrams
- Rehabilitation nursing guides
- NCLEX-style practice questions
These tools help future registered nurses review key concepts quickly and improve exam readiness.
Final Thoughts
Early mobility programs have transformed the way critically ill patients recover in the ICU. Rather than relying on prolonged bed rest, modern healthcare encourages safe movement as soon as patients are medically stable.
Because mobility improves muscle strength, respiratory function, and overall recovery, it has become an essential part of critical care nursing. The RN nurse plays a central role in assessing patient readiness, assisting with mobility activities, and ensuring patient safety throughout the process.
For students preparing for the NCLEX, understanding early mobility programs is an important aspect of modern patient care. With continued learning and the support of organized study tools like a nursing bundle, future registered nurses can develop the knowledge and confidence needed to support safe recovery for critically ill patients.