Deep vein thrombosis (DVT) is one of the most preventable yet potentially fatal conditions encountered in inpatient nursing. Every registered nurse must understand the mechanisms behind clot formation and the evidence-based interventions used to stop it — because DVT nursing prevention is not just a best practice, it is a patient safety imperative. On the NCLEX, DVT appears frequently across medical-surgical, critical care, and postoperative contexts. Mastering the pathophysiology and nursing care associated with DVT equips both student nurses and practicing RN nurses to act with precision and confidence at the bedside.
Virchow’s Triad: The Foundation of DVT Pathophysiology
To understand DVT, every nurse must first understand Virchow’s Triad — the three-factor framework that explains how thrombi form in the venous system. These three elements are:
- Venous stasis — slowed or pooling blood flow, most commonly seen in immobile or post-surgical patients
- Endothelial injury — damage to the inner lining of the vessel wall from trauma, surgery, or catheter insertion
- Hypercoagulability — an increased tendency of the blood to clot, associated with pregnancy, malignancy, inherited clotting disorders, or estrogen-containing medications
When one or more of these conditions exist, platelets and clotting factors aggregate within the deep veins — most commonly the femoral, popliteal, or iliac veins of the lower extremities. The resulting thrombus can partially or completely occlude venous return. If the clot breaks free, it becomes a pulmonary embolism (PE), a life-threatening emergency that nursing staff must be prepared to recognize and respond to immediately.
Risk Factors Every Nurse Must Recognize
Identifying patients at risk is the first step in DVT nursing prevention. High-risk populations include:
- Post-surgical patients, especially after orthopedic procedures (total hip or knee arthroplasty carries the highest DVT risk)
- Prolonged immobility — bed-bound patients, long-haul travelers, or those with stroke or spinal cord injury
- Pregnancy and the postpartum period — hormonal and mechanical factors both increase risk
- Malignancy — many cancers trigger hypercoagulable states
- Previous DVT or PE — prior history significantly elevates risk
- Obesity, dehydration, and smoking — all contribute to sluggish venous return and endothelial dysfunction
- Estrogen therapy or oral contraceptives — promote clotting factor synthesis in the liver
Standardized risk assessment tools such as the Caprini Risk Assessment Model are used in many facilities to stratify patients and guide prophylaxis decisions. The RN nurse plays a critical role in completing and acting on these assessments at admission.
Clinical Manifestations: What to Assess
DVT is often called a “silent” condition because it may be asymptomatic, particularly in the early stages. When symptoms are present, they typically include:
- Unilateral leg swelling — compare both extremities; even a 2 cm difference is clinically significant
- Redness, warmth, and tenderness along the affected vein
- Positive Homans’ sign — calf pain with dorsiflexion of the foot (note: this finding has low sensitivity and specificity and should not be used in isolation)
- Skin discoloration — the limb may appear dusky or cyanotic in severe cases
Nurses must also monitor for signs of pulmonary embolism, which include sudden-onset dyspnea, pleuritis chest pain, tachycardia, hypoxia, and hemoptysis. Any combination of these findings warrants immediate escalation using SBAR communication to the provider.
Diagnostic confirmation typically involves duplex ultrasonography, the gold standard for DVT diagnosis. Lab findings such as elevated D-dimer support clinical suspicion but are non-specific.
DVT Nursing Prevention: Evidence-Based Interventions
Prophylaxis is the cornerstone of DVT nursing prevention, and the registered nurse is responsible for implementing and monitoring these measures consistently.
Mechanical Prophylaxis:
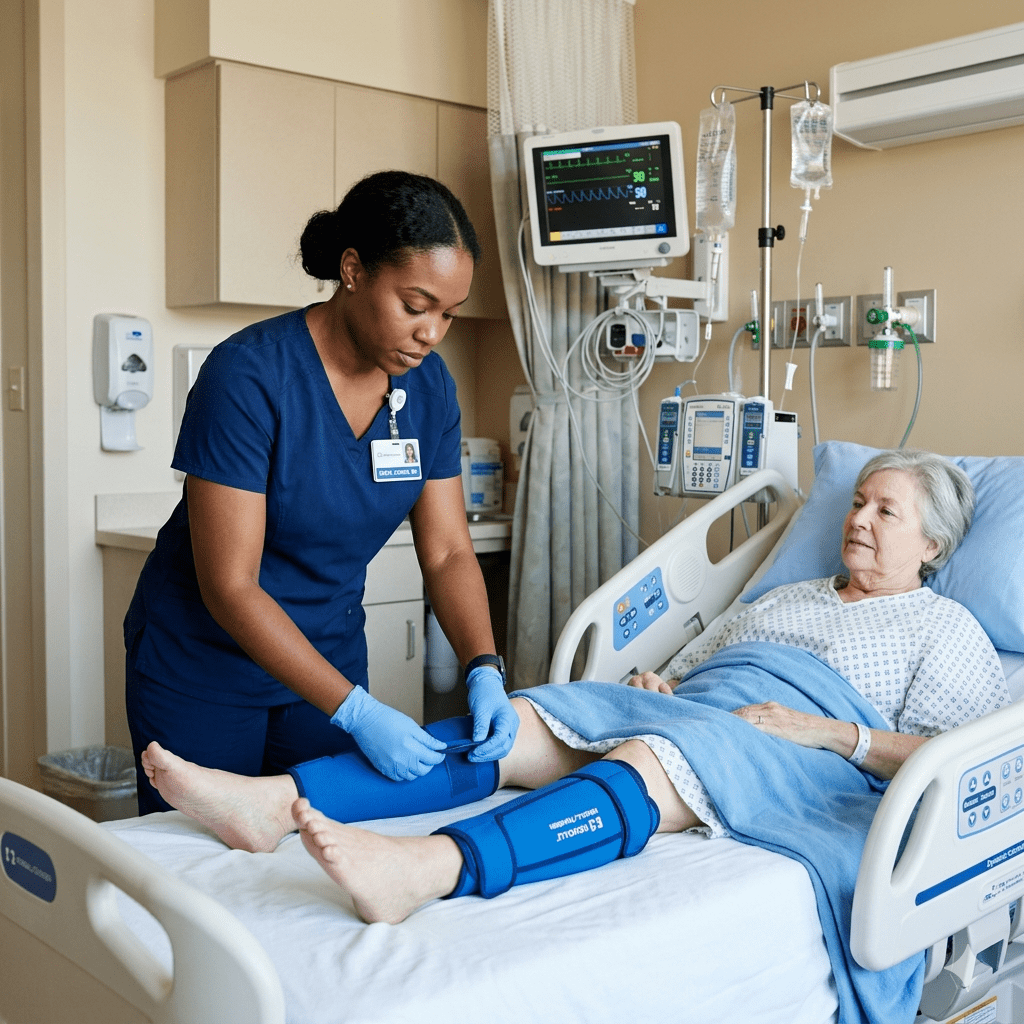
- Sequential compression devices (SCDs) — applied to the lower extremities, SCDs mimic the muscle pump action of ambulation, promoting venous return and reducing stasis. They should be worn continuously except during ambulation or skin assessment.
- Graduated compression stockings (TED hose) — used in moderate-risk patients to reduce venous pooling
Pharmacologic Prophylaxis:
- Unfractionated heparin (UFH) — commonly ordered as 5,000 units subcutaneously every 8–12 hours
- Low molecular weight heparin (LMWH) — agents such as enoxaparin (Lovenox) are preferred in many surgical and orthopedic protocols due to predictable dosing and reduced monitoring requirements
- Fondaparinux — a factor Xa inhibitor used in select patients
The RN nurse must reconcile anticoagulant orders carefully, monitor for signs of bleeding, and hold medications as ordered prior to invasive procedures.
Early Mobilization: Nursing research consistently demonstrates that early ambulation is one of the most effective DVT prevention strategies. Encouraging patients to get out of bed within hours of surgery — when clinically appropriate — significantly reduces venous stasis. Structured nursing care bundles that combine SCDs, anticoagulants, and ambulation protocols have been shown to reduce DVT incidence across medical-surgical units.
Hydration: Adequate fluid intake reduces blood viscosity and supports venous flow. Nurses should monitor intake and output, encourage oral hydration, and advocate for IV fluid orders in patients who are NPO or dehydrated.
Nursing Management of the Patient with Active DVT
When DVT is confirmed, the nursing focus shifts from prevention to treatment and complication monitoring. Key interventions include:
- Anticoagulation therapy — therapeutic anticoagulation is initiated, most commonly with IV heparin infusion titrated to maintain an aPTT 60–100 seconds, followed by transition to oral agents such as warfarin or direct oral anticoagulants (DOACs) like rivaroxaban (Xarelto) or apixaban (Eliquis)
- Limb elevation — elevating the affected extremity above heart level promotes venous drainage and reduces edema
- Pain management — analgesics are provided as ordered; document pain scores and response
- Bleeding precautions — all anticoagulated patients require close monitoring for hematuria, melena, gingival bleeding, or changes in mental status
- Patient education — the registered nurse must teach patients about the purpose of anticoagulation, the importance of follow-up INR monitoring (for warfarin), dietary considerations (e.g., vitamin K consistency), and signs of bleeding or clot recurrence to report
This nursing bundle of interventions — anticoagulation management, monitoring, elevation, pain control, and education — forms the standard of care for DVT across inpatient settings.
💡 NCLEX Tips for DVT
- SCDs should be applied before surgery and kept on continuously — remove only for ambulation or skin checks
- Heparin antidote = protamine sulfate; warfarin antidote = vitamin K (phytonadione)
- D-dimer is sensitive but not specific — an elevated result does not confirm DVT
- A patient on warfarin with a supratherapeutic INR (>3.0) requires priority nursing assessment for bleeding
- Homans’ sign is not reliable — always correlate with clinical picture and diagnostic imaging
Quick Reference: DVT Anticoagulants for NCLEX
| Drug | Class | Route | Monitoring | Antidote |
|---|---|---|---|---|
| Unfractionated Heparin | Anticoagulant | IV / SubQ | aPTT, platelet count | Protamine sulfate |
| Enoxaparin (Lovenox) | LMWH | SubQ | Anti-Xa level (select cases) | Protamine sulfate (partial) |
| Warfarin (Coumadin) | Vitamin K antagonist | PO | INR (goal 2–3) | Vitamin K, FFP |
| Rivaroxaban (Xarelto) | Factor Xa inhibitor | PO | None routinely | Andexanet alfa |
| Apixaban (Eliquis) | Factor Xa inhibitor | PO | None routinely | Andexanet alfa |
Conclusion
DVT remains one of the most significant preventable threats to hospitalized patients, and the registered nurse is the last and most consistent line of defense. From identifying Virchow’s Triad during pathophysiology review to applying SCDs, administering anticoagulants safely, and educating patients before discharge, DVT nursing prevention requires clinical knowledge, systematic assessment, and proactive intervention. Whether preparing for the NCLEX or refining bedside practice, mastering this content is essential for every RN nurse. Reinforce your knowledge with practice questions at rn-nurse.com/nclex-qcm/ and explore the full nursing bundle of study resources at rn-nurse.com/nursing-courses/ to strengthen your exam readiness today.