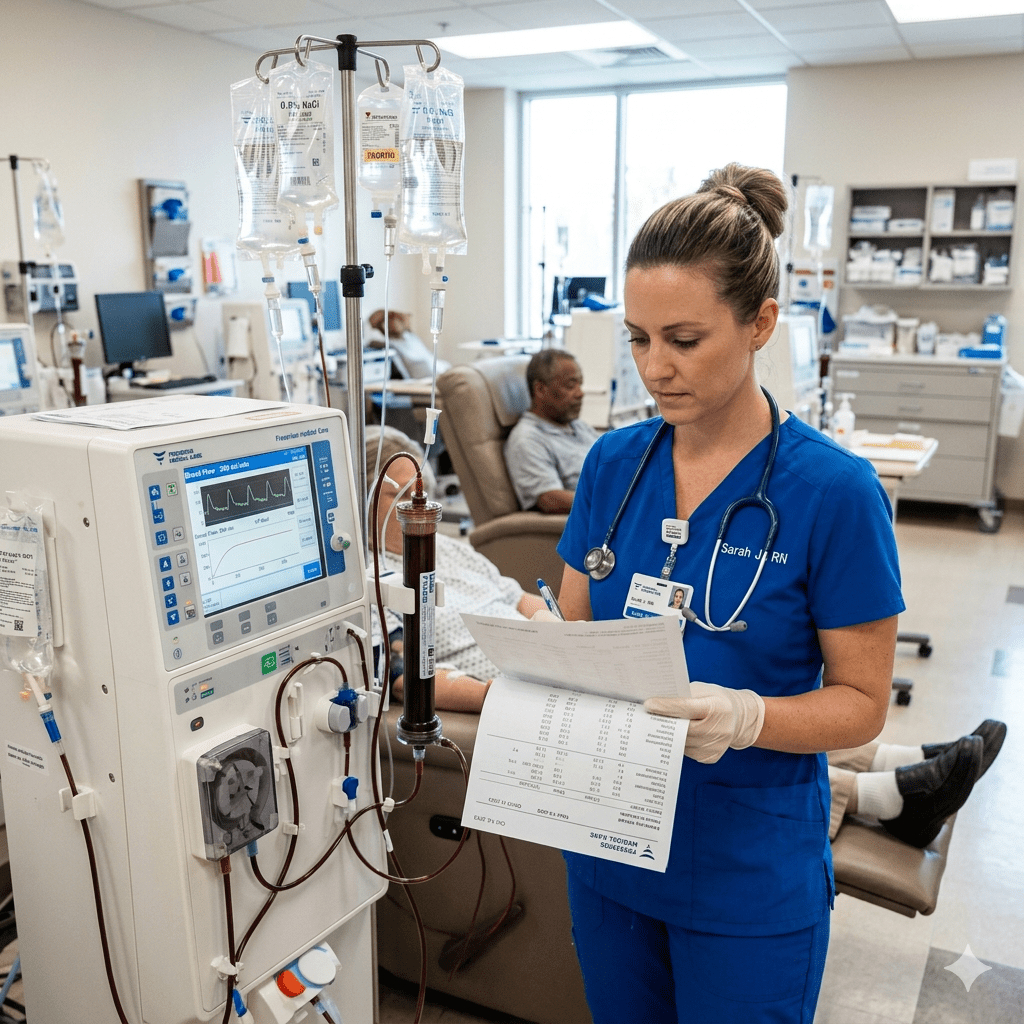
Dialysis fundamentally alters the body’s fluid and electrolyte balance — and for the registered nurse managing these patients, vigilance is not optional. Electrolyte monitoring during dialysis is one of the highest-acuity responsibilities in nephrology and critical care nursing, with life-threatening imbalances capable of developing within hours. Whether caring for a patient on hemodialysis (HD) or peritoneal dialysis (PD), the RN nurse must understand which electrolytes shift, why they shift, and what to do when values fall outside safe parameters. This topic is also consistently tested on the NCLEX, making it essential for any nursing student preparing for licensure.
Why Electrolyte Monitoring During Dialysis Matters
The kidneys regulate six major electrolytes: potassium, sodium, calcium, phosphorus, magnesium, and bicarbonate. When renal failure occurs, these mechanisms fail — and dialysis serves as an artificial substitute. However, dialysis is an imperfect replacement. The dialysate (the fluid used to draw out waste) can pull out electrolytes too aggressively or not aggressively enough, depending on its composition and the patient’s current serum levels.
A registered nurse must understand that both hemodialysis and peritoneal dialysis carry distinct risks. Hemodialysis causes more rapid fluid and electrolyte shifts over a 3–4 hour session. Peritoneal dialysis is slower and continuous, creating more gradual but equally important changes. In both cases, nursing assessment before, during, and after treatment is the cornerstone of safe care.
Key Electrolytes to Monitor and Their Normal Ranges
The following electrolytes are most affected by dialysis. Every RN nurse and nursing student should have these ranges memorized — they appear frequently on the NCLEX.
| Electrolyte | Normal Range | Dialysis Risk |
|---|---|---|
| Potassium (K⁺) | 3.5–5.0 mEq/L | Hyperkalemia pre-dialysis; hypokalemia post |
| Sodium (Na⁺) | 136–145 mEq/L | Hypo- or hypernatremia depending on fluid shifts |
| Calcium (Ca²⁺) | 8.5–10.5 mg/dL | Hypocalcemia due to impaired vitamin D activation |
| Phosphorus | 2.5–4.5 mg/dL | Hyperphosphatemia from dietary intake and renal failure |
| Magnesium (Mg²⁺) | 1.5–2.5 mEq/L | Hypermagnesemia, especially with magnesium-containing antacids |
| Bicarbonate (HCO₃⁻) | 22–26 mEq/L | Metabolic acidosis pre-dialysis; correction post-treatment |
Nurses should obtain baseline labs before each dialysis session and reassess post-treatment, particularly for potassium and calcium.
Potassium: The Most Dangerous Electrolyte Shift in Dialysis Patients
Hyperkalemia is the most immediately life-threatening electrolyte imbalance in dialysis patients and a classic NCLEX focus. Patients with end-stage renal disease (ESRD) cannot excrete potassium normally, leading to dangerous accumulation — particularly between dialysis sessions. Serum potassium above 6.0 mEq/L requires urgent intervention.
Signs of hyperkalemia include:
- Peaked T waves on EKG (first and most reliable ECG change)
- Muscle weakness progressing to flaccid paralysis
- Bradycardia and potentially fatal arrhythmias
- Nausea and abdominal cramping
Nursing interventions for hyperkalemia include:
- Restricting dietary potassium (avoid bananas, oranges, potatoes, tomatoes)
- Administering sodium polystyrene sulfonate (Kayexalate) as ordered to bind potassium in the GI tract
- Preparing for urgent dialysis if arrhythmias develop
- Continuous cardiac monitoring
Post-dialysis, the nurse must assess for hypokalemia (K⁺ < 3.5 mEq/L), which can also cause arrhythmias, weakness, and constipation.
Calcium and Phosphorus: An Interdependent Imbalance
Dialysis patients frequently develop hypocalcemia and hyperphosphatemia simultaneously — a consequence of impaired renal activation of vitamin D and phosphate retention. These two electrolytes have an inverse relationship: as phosphorus rises, calcium falls.
The registered nurse must monitor for signs of hypocalcemia, including:
- Chvostek’s sign (facial twitch with tapping over the facial nerve)
- Trousseau’s sign (carpal spasm with blood pressure cuff inflation)
- Muscle cramps, tetany, and in severe cases, seizures
Nursing interventions include:
- Administering calcium carbonate or calcium acetate with meals (acts as a phosphate binder)
- Ensuring prescribed vitamin D analogs (e.g., calcitriol, paricalcitol) are given
- Teaching patients to limit phosphorus-rich foods: dairy, nuts, cola beverages, processed meats
This electrolyte pair is a staple of the NCLEX renal section, and mastering it as part of a nursing bundle review will significantly improve exam readiness.
Sodium and Fluid Balance Considerations
Sodium regulation in dialysis patients is closely tied to fluid management. These patients are typically on strict fluid restrictions — often 1,000–1,500 mL/day — to prevent fluid overload between sessions.
Hyponatremia (Na⁺ < 136 mEq/L) in dialysis patients often reflects dilutional hyponatremia — too much fluid rather than true sodium depletion. Signs include confusion, headache, nausea, and in severe cases, seizures.
Hypernatremia (Na⁺ > 145 mEq/L) is less common but can occur if the dialysate sodium concentration is too high. Symptoms include intense thirst, agitation, dry mucous membranes, and neurological changes.
The RN nurse should monitor daily weights, assess for edema, and document fluid intake and output meticulously. A weight gain of more than 1–2 kg between dialysis sessions signals concerning fluid retention and must be reported promptly.
Bicarbonate and Acid-Base Correction in Dialysis
Patients with ESRD commonly present with metabolic acidosis — the kidneys’ inability to excrete hydrogen ions leads to a drop in serum bicarbonate. Patients may exhibit Kussmaul breathing, fatigue, confusion, and decreased cardiac contractility.
Dialysis corrects metabolic acidosis by delivering a bicarbonate-enriched dialysate that diffuses into the blood, raising serum HCO₃⁻ levels toward normal. The nursing role includes:
- Monitoring arterial blood gases (ABGs) or venous CO₂ levels pre- and post-treatment
- Assessing respiratory compensation (rate and depth of breathing)
- Recognizing signs of overcorrection — metabolic alkalosis can cause tetany and cardiac irritability
A comprehensive nursing bundle that includes acid-base interpretation alongside electrolyte content will help nurses and students master this complex interplay.
💡 NCLEX Tips for Electrolyte Monitoring During Dialysis
- Peaked T waves are the earliest EKG sign of hyperkalemia — always select this on NCLEX before other findings.
- Chvostek’s and Trousseau’s signs indicate hypocalcemia — dialysis patients are at high risk.
- Weigh patients before and after dialysis — this is the most accurate measure of fluid removal.
- Hold antihypertensives before dialysis unless ordered otherwise — BP can drop severely during treatment.
- Calcium carbonate is given WITH meals to bind dietary phosphorus — not between meals.
Pre- and Post-Dialysis Nursing Assessment
A systematic nursing assessment protects the patient at every stage of treatment.
Pre-dialysis:
- Obtain serum electrolytes, BUN, creatinine, and weight
- Assess vascular access (AV fistula, graft, or central venous catheter) for patency, thrill, and bruit
- Review current medications — hold nephrotoxic agents and water-soluble vitamins (removed by dialysis)
During dialysis:
- Monitor vital signs every 30–60 minutes
- Assess for disequilibrium syndrome: headache, nausea, and confusion caused by rapid fluid and electrolyte shifts
- Watch for signs of air embolism (a rare but emergent complication): chest pain, dyspnea, cyanosis
Post-dialysis:
- Recheck electrolytes and compare to pre-treatment values
- Assess access site for bleeding or hematoma
- Educate patient on dietary restrictions and fluid limits before the next session
Conclusion
Electrolyte monitoring during dialysis is a high-stakes, high-frequency nursing responsibility that demands both clinical precision and proactive assessment. From managing life-threatening hyperkalemia to detecting subtle calcium-phosphorus imbalances, the registered nurse serves as the critical link between the dialysis machine and patient safety. These concepts are not only foundational to nephrology nursing practice — they are consistently tested on the NCLEX. Strengthen your knowledge base with targeted practice questions and a structured nursing bundle that covers renal and electrolyte topics in depth.
Practice NCLEX-style dialysis questions at rn-nurse.com/nclex-qcm/ and explore the full electrolyte nursing courses at rn-nurse.com/nursing-courses/.